30 Most Common Questions About Standard First Aid Training and Certification
First aid and CPR training are essential skills that empower individuals to respond effectively in emergencies. The Canadian Red Cross Standard First Aid (also known as Intermediate First Aid) course is a cornerstone of this preparedness, offering comprehensive skills to manage a wide array of medical emergencies and injuries. If you’re considering getting certified, or if your workplace requires it, here are 30 of the most frequently asked questions, with comprehensive answers and reasons to choose Safe + Sound First Aid Training in the Metro Vancouver and Tri-Cities area.
General Information & Benefits
Q1: What is Standard First Aid certification?
A1: Standard First Aid (SFA) is a comprehensive first aid and CPR course developed by the Canadian Red Cross. It provides participants with the knowledge and skills to recognize and respond to a wide range of first aid emergencies, from minor injuries to life-threatening conditions. It includes CPR training for adults, children, and infants, and how to use an Automated External Defibrillator (AED).
Q2: What are the main benefits of taking a Canadian Red Cross Standard First Aid course from a recognized Red Cross Training Partner like Safe + Sound First Aid Training?
A2: The benefits are extensive, ranging from personal empowerment to professional advantage. You gain:
- Life-Saving Skills: The ability to provide critical care until professional medical help arrives.
- Confidence in Crisis: Training reduces panic and equips you to act decisively and effectively.
- Workplace Compliance: Meets numerous regulatory requirements across various industries.
- Community Safety: You become a valuable asset capable of assisting in public emergencies.
- Peace of Mind: Knowing you can protect yourself and your loved ones.
- Career Advancement: Many employers prioritize candidates with recognized first aid certification.

Q3: What specific topics are covered in a Standard First Aid course?
A3: A Standard First Aid course offers in-depth coverage of:
- The Responder: Legalities, consent, personal safety, infection prevention.
- Responding to Emergencies: Check, Call, Care system, activating EMS.
- Airway, Breathing, and Circulation (ABCs).
- Cardiopulmonary Resuscitation (CPR) for adults, children, and infants (CPR Level C).
- Automated External Defibrillator (AED) use.
- Choking (adult, child, infant).
- Sudden Medical Conditions: Heart attack, stroke, diabetes, seizures, anaphylaxis, shock.
- Wounds and Bleeding: Management of various types of soft tissue injuries and severe bleeding.
- Head, Neck, and Spinal Injuries: Recognition and stabilization.
- Bone, Muscle, and Joint Injuries: Fractures, sprains, dislocations, and immobilization.
- Environmental Emergencies: Heat/cold exposure (heat stroke, hypothermia, frostbite).
- Poisons: Recognition and initial care.
Q4: How does Standard First Aid differ from Emergency First Aid?
A4: The key differences lie in duration and scope:
Emergency First Aid (EFA): A shorter (approx. 6-8 hours, 1 day) course focused on immediate, life-threatening emergencies. It covers basic CPR, choking, severe bleeding, and the Check, Call, Care system.
Standard First Aid (SFA): A more comprehensive (approx. 14-16 hours, 2 days) course that includes all EFA topics plus extensive training on medical conditions, bone/muscle/joint injuries, head/neck/spinal injuries, environmental emergencies, and poisons, providing a broader skillset and deeper understanding.
Q5: What is CPR Level C, and why is it included in Standard First Aid?
A5: CPR Level C is the most comprehensive CPR certification for lay rescuers. It teaches resuscitation skills (chest compressions and rescue breaths) for adults, children, and infants, along with the use of an AED for all age groups. It’s included in Standard First Aid to ensure participants are prepared to respond to cardiac emergencies across the entire age spectrum, making the certification highly versatile and applicable in diverse situations.
Who Needs Certification & Recognition
Q6: Who is the Standard First Aid course designed for?
 A6: This course is ideal for a wide range of individuals:
A6: This course is ideal for a wide range of individuals:
- Designated Workplace First Aid Attendants: Fulfills many employer requirements.
- Child Care Workers & ECE Students: Accepted for licensing in many contexts (see Q9).
- Adult Care Providers: Essential for those in community care settings (see Q10).
- Teachers and School Staff: To manage emergencies involving students.
- Coaches & Sports Instructors: To handle sports-related injuries.
- Construction & Industrial Workers: For higher-risk work environments.
- Parents & Guardians: To protect their families effectively.
- Community Volunteers: Enhances safety at events and in groups.
- Anyone seeking comprehensive preparedness: For personal readiness at home or in public.
Q7: Is Canadian Red Cross Standard First Aid recognized by WorkSafeBC?
A7: Yes. WorkSafeBC officially recognizes the Canadian Red Cross Standard First Aid with CPR Level C. It is accepted as equivalent to Intermediate First Aid (formerly OFA Level 2) under the new CSA-aligned standards, depending on the workplace hazard assessment. It exceeds the training requirements for Basic First Aid, formerly Occupational First Aid Level 1 (OFA Level 1)
Q8: Is Standard First Aid acceptable for BC Child Care Licensing?
A8: Yes. While the Canadian Red Cross also offers an “Emergency Child Care First Aid & CPR Level B” course specifically for childcare, the Canadian Red Cross Standard First Aid & CPR Level C is widely accepted by BC Child Care Licensing. It is often preferred or required for childcare workers who care for older children (aged eight and above) as well as babies and younger children, due to its more comprehensive coverage.
Q9: Is this course recognized for BC Adult Care (Community Care) licensing?
A9: Yes. Standard First Aid, with its in-depth coverage of various medical conditions and adult-specific emergencies, typically meets or exceeds the first aid training requirements for licensed adult care and community care facilities operating under the BC Ministry of Health’s Community Care and Assisted Living Act.
Q10: Can parents and the general public benefit from Standard First Aid, even without a specific job requirement?
A10: Definitely! Parents gain crucial skills for responding to choking, fevers, injuries, or sudden illnesses in children and infants. For the general public, it offers immense peace of mind, knowing they can effectively help family, friends, or strangers during emergencies at home, work, or in public settings. It transforms bystanders into lifesavers. Source: prosafetraining.ca
Course Logistics & Certification 
Q11: What is the typical duration of a Standard First Aid course?
A11: A full Canadian Red Cross Standard First Aid course is typically 14-16 hours in duration. This is often split into an online component and an in-person practical session, known as blended training. You can find more information about how blended Standard First Aid training works here.
Q12: Is there an online component for Standard First Aid training?
A12: Yes, many Canadian Red Cross providers, including Safe + Sound First Aid Training, offer Standard First Aid in a blended learning format. This means you complete a significant portion of the theoretical content (typically 6-8 hours) online at your own pace before attending a mandatory in-person practical session.
Q13: How long is the in-person component of a blended Standard First Aid course?
A13: The mandatory in-person practical session for a blended Standard First Aid course typically lasts 8 hours. It is conducted in a single, full-day session, including breaks. This session is dedicated to hands-on skill practice, scenario drills, and practical assessment under the direct supervision of a certified instructor.
Q14: How long is the Standard First Aid certificate valid?
A14: Canadian Red Cross Standard First Aid certificates are valid for three years from the date of issue.
Q15: What are the requirements for Standard First Aid recertification?
A15: To recertify, you must:
- Possess a current, unexpired Canadian Red Cross Standard First Aid & CPR Level C certificate.
- Complete a shorter recertification course (typically 6-8 hours) before your current certificate expires.
- Demonstrate continued proficiency in all required practical skills and pass a written exam.
If your certificate expires, you will generally need to retake the full Standard First Aid course.
Q16: What should I expect during the in-person class?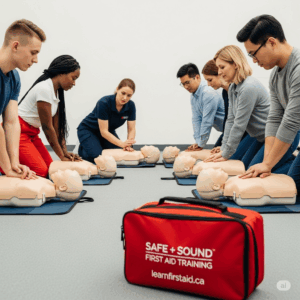
A16: You can expect an engaging and hands-on learning experience. The instructor will guide you through practical scenarios, demonstrations, and skill practice using manikins and first aid equipment. You’ll practice CPR, choking rescues, bandaging, splinting, and patient assessment. Active participation and skill demonstration are key.
Q17: Does Standard First Aid include a written exam?
A17: Yes, most Canadian Red Cross Standard First Aid courses include a written knowledge evaluation (exam) in addition to the practical skills assessment. The test is usually in a multiple choice format. A minimum passing grade (often 75%) is usually required for certification.
Q18: What is the typical cost of a Standard First Aid course in BC?
A18: The cost of a Standard First Aid course in BC can vary depending on the provider and format (blended vs. in-class). Generally, prices range from approximately $170 to $200+ GST for the full course. Recertification courses are typically less. Some course providers, like Safe + Sound First Aid Training, provide a CPR pocket mask included in the price.
Q19: Can I get private group training for my workplace or organization?
A19: Yes, most reputable first aid training providers, including Safe + Sound First Aid Training, offer private group training options. This allows organizations to train their staff at their facility (if suitable) or at the training provider’s location, with customized scheduling.
Practical Considerations & Maintenance
Q20: What kind of first aid kit should a certified first aider have?
A20: While the course doesn’t certify you to be a workplace first aid kit expert, it prepares you to use everyday items. For personal use, a well-stocked basic kit should include bandages (adhesive, gauze, triangular), antiseptic wipes, medical tape, sterile gauze pads, gloves, scissors, tweezers, a CPR mask with a one-way valve, and an emergency blanket. Workplaces will have specific WorkSafeBC compliant kits.
Q21: How can I maintain my first aid skills between recertifications?
A21:
- Review Course Materials: Periodically re-read your manual or access online resources.
- Practice Skills: If you have access to manikins or willing volunteers, practice CPR compressions and rescue breaths.
- Stay Informed: Follow reputable first aid organizations for updates and tips.
- Review Scenarios: Mentally walk through how you would respond to different emergencies.
- Consider Higher-Level Training: If applicable, take an advanced course.
Q22: What are the legal responsibilities of a first aider in Canada?
A22: In Canada, “Good Samaritan” laws generally protect individuals who provide voluntary emergency first aid in good faith, without expectation of reward, and gross negligence. Your primary responsibilities include acting within the scope of your training, obtaining consent (if the person is conscious), calling for professional medical assistance, and providing ongoing care until relieved by EMS or a higher-trained professional.
Q23: Are there any prerequisites for taking a Standard First Aid course?
A23: Generally, there are no prerequisites for taking a full Canadian Red Cross Standard First Aid course. The course is designed for individuals with no prior first aid knowledge. However, for recertification courses, a valid, non-expired previous certification is required.
Q24: What if I have a disability or a medical condition? Can I still take the course?
A24: Most providers strive to be inclusive. If you have a disability or medical condition that may affect your ability to perform specific physical skills (such as CPR compressions on the floor), it’s best to contact the training provider in advance. They can discuss accommodations or alternative assessment methods to ensure you can participate safely and effectively.
Q25: What should I wear to a first aid class?
A25: Wear comfortable, loose-fitting clothing that allows for movement. You’ll be performing hands-on skills, including kneeling, bending, and potentially lying on the floor for CPR practice. Closed-toe shoes are also recommended.
Q26: What kind of certification will I receive?
A26: Upon successful completion, you will receive a digital Canadian Red Cross Standard First Aid & CPR Level C with AED certification. This is a nationally recognized certification, valid for three years from the date of issue.
Q27: Can I upgrade my Emergency First Aid to Standard First Aid?
A27: No, you cannot simply “upgrade” an Emergency First Aid certificate to a Standard First Aid certificate. To obtain Standard First Aid certification, you must take the full Standard First Aid course, even if you already hold an EFA certificate. This is because SFA covers significantly more material and requires more in-person practice hours.
Q28: What is the difference between CPR-A, CPR-B, and CPR-C?
A28: These levels refer to the age groups covered for CPR and AED training:
CPR-A: Adult CPR and AED.
CPR-B: Child and infant CPR and AED (primarily for childcare, often included in Emergency Child Care First Aid).
CPR-C: Adult, child, and infant CPR and AED. This is the most comprehensive level for the general public, typically included in Standard First Aid.
Note: There is also BLS (Basic Life Support) for healthcare providers, which is a higher level.
Q29: Are there any specific things I need to prepare before the blended learning class?
A29: Yes, for blended learning, you must complete the online self-study theory component before your scheduled in-person practical session. Your provider will send you instructions and a link to access the online material. Failure to complete this prerequisite usually means you will not be admitted to the in-person class and may forfeit your registration fee.
Q30: Why is it important to learn first aid from a reputable organization like the Canadian Red Cross?
A30: Learning from a recognized organization like the Canadian Red Cross ensures that your training is:
- Evidence-Based: Based on the latest scientific guidelines and best practices.
- Nationally Recognized: Your certification will be accepted by employers and regulatory bodies across Canada.
- Standardized: Ensures consistent, high-quality instruction regardless of where you take the course.
- Trusted: The Red Cross has a long history of humanitarian service and emergency preparedness, lending credibility to your certification. Source: Canadian Red Cross, Acticert.com
Why Choose Safe + Sound First Aid Training Ltd. for Your Standard First Aid in Metro Vancouver and the Tri-Cities?

When it comes to acquiring life-saving skills, the choice of your training provider is as crucial as the course itself. For residents and professionals in Metro Vancouver and the Tri-Cities area (Coquitlam, Port Coquitlam, Port Moody), Safe + Sound First Aid Training Ltd. (www.learnfirstaid.ca) stands out as an exceptional choice for your Canadian Red Cross Standard First Aid certification.
Here’s why choosing Safe + Sound offers distinct advantages:
Unwavering Credibility and Proven Experience:
Proud Canadian Red Cross Training Partner: This isn’t just a label; it means Safe + Sound adheres to the highest national standards set by the Canadian Red Cross. Your certification will be universally recognized and trusted by employers, WorkSafeBC, BC Child Care Licensing, and BC Adult Care Licensing.

Industry experience: Established in 1999, with over 25 years in the industry, Safe + Sound brings a depth of experience that ensures robust, effective training. The company adheres to the best practices in first aid education.
Award-Winning Excellence: As the first Canadian recipient of the Red Cross Partners in Humanity Citation, Safe + Sound’s commitment to humanitarian principles and quality instruction is formally acknowledged.
Excellent reputation: A+ Better Business Bureau rating and 4.8/5 Google rating: This reflects a strong track record of customer satisfaction and ethical business operations.
50,000+ Clients Trained: This vast experience means they understand diverse learning needs and can effectively guide you to proficiency.
A Passionate, Purpose-Driven Approach:
Safe + Sound’s foundation is built on a profound personal experience – their founder’s friend’s baby nearly choked, highlighting the critical need for first aid skills. This isn’t just a business; it’s a mission to empower people and build safer communities. This passion translates directly into dedicated, high-quality instruction.
Expert Instructors Focused on Confidence and Application:
Their instructors are not only certified but also experienced professionals who are passionate about teaching. They bring real-world knowledge and focus on ensuring you leave not just with a certificate, but with the confidence and practical skills to effectively apply your knowledge in real emergencies. They prioritize hands-on practice, which is vital for retaining life-saving techniques.
Optimal Learning Environment and Convenience:
Coquitlam Classroom: Safe + Sound offers convenient public classes at their Coquitlam classroom. This location is easily accessible for residents across the Tri-Cities and surrounding Metro Vancouver areas (like Burnaby, New Westminster, Surrey, Langley, Pitt Meadows, and Maple Ridge), featuring ample free parking and proximity to public transit (bus and SkyTrain).
Flexible Blended Learning: Their popular blended format allows you to complete the theoretical component online at your own pace, reducing in-class time and offering greater scheduling flexibility.
High-Quality Equipment: You’ll train with up-to-date manikins and first aid equipment, ensuring a realistic and effective learning experience. 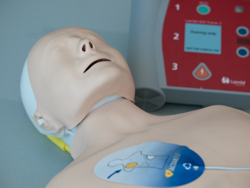
Tailored Solutions for Groups and Organizations:
For businesses, childcare centres, schools, and other organizations in Metro Vancouver, Safe + Sound offers private group training. They can deliver the Standard First Aid course directly at your facility (if suitable) or at their Coquitlam classroom, allowing for customized scheduling and content relevant to your specific workplace or group needs. This is ideal for ensuring all staff are compliant and trained together.
Comprehensive Support and Resources:
Safe + Sound provides clear communication regarding course prerequisites (like completing the online component for blended learning), ensuring you are well-prepared for your class.
Their commitment extends beyond the classroom, evidenced by positive testimonials from diverse clients, including parents, professionals, and community leaders.
By choosing Safe + Sound First Aid Training, you’re not just registering for a course; you’re investing in a legacy of excellence, genuine passion for safety, and an unparalleled learning experience that will equip you to make a difference when it matters most. Take the proactive step today and empower yourself with the vital skills of a confident first responder.
Register for your Canadian Red Cross Standard First Aid class with Safe + Sound First Aid Training at learnfirstaid.ca and become a vital link in the chain of survival in your community.
Learn to save a life.





 A6: This course is ideal for a wide range of individuals:
A6: This course is ideal for a wide range of individuals:












